Diabetic foot ulcers are wounds that occur on the feet of people with diabetes. A multi-disciplinary approach is important because this is a complex problem. Usually, diabetic foot ulcers start with neuropathy which is nerve damage from higher sugar levels.
What are Diabetic Foot Ulcers?
Diabetic foot ulcers are wounds that occur on the feet of people with diabetes. They can be the result of trauma/injury or other reasons. Sometimes with a deformity of the foot, like with a bunion or hammertoe, there may exist increased pressure on the shoe, which can lead to breakdown of the skin.
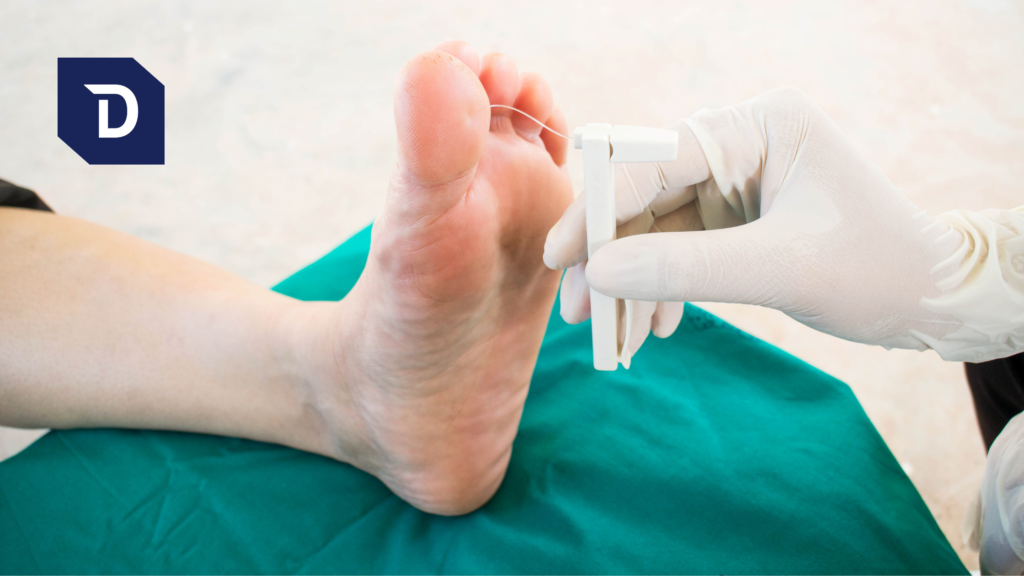
Neuropathy leads to loss of protective sensation and increased risk of trauma. The trauma may be from something as simple as a minor cut or blister that goes unnoticed until it becomes infected. Protective sensation is the minimal amount of sensation required to let the patient know that something abnormal is occurring in the foot. If the patient with neuropathy is unable to detect pain in the foot, he may have a pebble or some other foreign body in the shoe all day long without knowing it.
Patients with diabetic neuropathy also can have extremely dry skin. The reason for this is not because they are inadequately hydrated. There is an interesting connection between the nervous system and the skin. Every sebaceous gland has some smooth muscle which needs to receive a stimulus from a nerve. If the nerve is not working adequately because of neuropathy, the stimulus to secrete sweat will not occur. The consequence of inadequate sweat secretion is dry skin. Drier skin is more susceptible to breakdown, ulceration, and infection.

How serious is a diabetic ulcer on the foot?
Diabetic foot ulcers are a serious complication of diabetes and can lead to serious infections, amputation, and even death. The constant pressure of walking and standing can cause the ulcer to become larger and deeper, making it difficult for the wound to heal. If left untreated, diabetic ulcers can become infected, whether this is a soft tissue skin infection or a deeper bone infection. Early diagnosis and treatment are essential for preventing serious complications from diabetic ulcers.
Here is a scary statistic. If a diabetic ends up with a higher amputation (below-knee or above-knee amputation), the 5-year survival rate is lower compared to some of the worst types of cancers.
What are the signs of infection in diabetic foot?
Fortunately, several early warning signs can indicate an infection is present. These include redness, pain, warmth, increased drainage, and swelling. If you notice any of these signs, it is important to see a doctor immediately. With prompt treatment, many diabetic foot infections can be successfully resolved without causing long-term damage.
How do you fix poor blood circulation?
Poorly controlled diabetes can be a risk factor for reduced circulation in the legs. This is known as peripheral vascular disease. Diabetics will have clogged arteries mostly in the tibial vessels which means that the reduced blood flow typically occurs in the arteries past the knee. Without adequate circulation, it is more challenging for nutrients and oxygen to reach the ulceration so that it can progress to the normal healing cycle. Blood flow must be assessed with a diabetic foot ulcer. There are a few ways to do this. The simplest way is to check pulses on examination. Two main arteries can be assessed in the foot. The first is on top of the foot and is called the dorsalis pedis artery. The other artery is behind the inner part of the ankle and is called the posterior tibial artery. More quantitative assessments can be performed through a vascular lab. This is referred to as noninvasive testing. If blood flow is insufficient for healing, it is recommended that the patient undergo evaluation by either a vascular surgeon or interventional radiologist. Typically, the first step is to have a procedure known as an angiogram. This is a minimally invasive procedure that allows the blood flow to be visualized with IV contrast material. If any significantly narrowed vessels are identified, they can be addressed with either balloon angioplasty or stenting of the vessel. Sometimes these minimally invasive procedures are inadequate or not the correct procedure to do. A bypass would have to be considered and this is a procedure performed by a vascular surgeon.
What is offloading in podiatry?
It is important to reduce the pressure on an ulcer while it heals. Any undue pressure will interfere with the healing process and possibly lead to an increase in the size of the ulceration. There are a few ways to offload an ulcer on the bottom of the foot. Examples would include offloading felt, surgical shoes, cam boots, total contact casting, and external fixation.
Surgery can also be utilized to offload an ulcer. One of the most relevant examples would be when there is an ulcer at the tip of one of the toes. These are extremely difficult to heal especially in the setting of toe contracture/a hammertoe. A very effective procedure, in this case, is to release the flexor tendon on the bottom of the toe that is causing the contracture. The tendon is completely transected and allows the toe to straighten out again. This leads to the tip of the toe no longer making forceful contact with the ground and allows the ulceration to heal.
We have had many successful outcomes with this tendon release procedure known as a flexor tenotomy. I recall one patient that had an ulcer for more than one year (one of many examples). I was becoming concerned because the ulcer was around for so long and was getting very close to the bone at the tip of the toe. A flexor tenotomy was recommended and performed. The patient’s ulceration healed in less than 1 week.
How to optimize the healing of a diabetic foot ulcer
The first step in managing a diabetic foot ulcer is to control the infection. This usually requires antibiotics given either orally or intravenously. If the infection is not controlled, it can lead to sepsis which is a life-threatening condition caused by bacteria in the bloodstream.
The third step in managing a diabetic foot ulcer is to promote healing. This can be done with local wound care including cleansing the wound, removing dead tissue (debridement), and applying dressings. If the wound does not heal with local wound care, other options such as negative pressure therapy or skin grafts may be necessary.
The management of diabetic foot ulcers requires a multidisciplinary team including wound care specialists, podiatrists, endocrinologists, and infectious disease specialists. The goals of treatment are to control the infection, relieve pain, promote healing, and prevent amputation.
The fourth step in managing a diabetic foot ulcer is to prevent amputation. Amputation may be necessary if the infection cannot be controlled or if the wound does not heal despite aggressive treatment. Prevention of amputation starts with early recognition and treatment of diabetic foot ulcers. It is also important to keep your feet clean and dry, wear appropriate shoes, and check your feet daily for any new wounds or changes in existing wounds.
Prophylatic Diabetic Foot Surgery – what is it?
Preventive or prophylactic surgery is any operation performed to prevent the future occurrence of disease or deformity. In the case of diabetic foot surgery, it is typically performed to prevent ulceration and subsequent complications such as infection, which can lead to serious health issues including amputation. There are many different types of prophylactic diabetic foot surgeries, including procedures to correct bunions and hammertoes. These surgeries usually involve the removal of bone or other tissue to straighten the toe and reduce pressure on the foot. In some cases, surgery may also be performed to release tightened ligaments or tendons. While prophylactic diabetic foot surgery can be beneficial in preventing ulceration and infection, it is important to note that it is not always successful in preventing these complications. Surgery is typically reserved for patients who have already developed bunions or hammertoes and are at high risk for ulceration. Patients should talk to their doctor about their specific risks and whether prophylactic surgery is right for them.
Diabetic foot ulcers are wounds that occur on the feet of people with diabetes mellitus and can lead to serious complications if left untreated. Early recognition and treatment of diabetic foot ulcers are essential to avoid more serious problems such as infection or amputation. If you have diabetes mellitus, it is important to check your feet daily for any new wounds or changes in existing wounds so that they can be treated promptly by your healthcare team.
Dr. Nodelman is an experienced foot and ankle provider heavily involved in the treatment of lower extremity ulcers and diabetic foot ulcers. He is a member of the Inova Fairfax Medical Campus emergency call service for foot and ankle issues including emergencies related to the diabetic foot. He also sees patients at the Inova Wound Healing Center.

