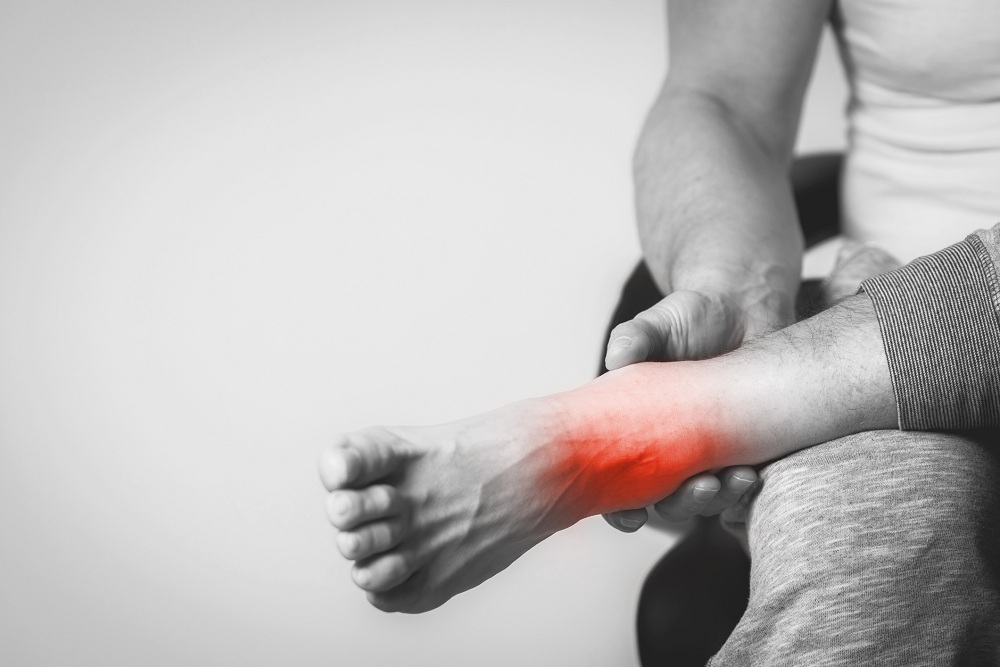
If you are experiencing inner ankle pain, it could be your posterior tibial tendon. When it becomes damaged, it can cause sharp pains in your inner ankle or your arch. It can also feel like it is popping and be sore when you touch it. These are all signs of posterior tibial tendonitis. It commonly occurs in runners.
Diagnosing the Problem
It is important to have any foot or ankle pain looked at. Certain symptoms can manifest in various ailments. You want the correct diagnosis so you can get the proper treatment. When you make an appointment, we go over your symptoms and examine your foot. We will order CT or MRI scans if needed. Possible treatments include:
- In-home stretches
- Physical therapy
- Anti-inflammatory medication
- Orthotics
- Bracing or a cam boot if needed
- Radial Shockwave Treatment
- Platelet-Rich plasma injections
- Surgery
When Can I Start Running Again?
Posterior tibial tendonitis doesn’t just cause inner ankle pain; it can do serious damage. You need to take care of your foot and allow it to heal. You will want to return to running slowly. So yes, inner ankle pain could be the posterior tibial tendon.
Posterior Tibial Tendonitis is an overuse injury that occurs when the posterior tibial tendon, which connects to a bone called the “navicular” in the foot, becomes overworked and inflamed. It is commonly seen in runners and athletes who engage in high-impact activities, as well as those who have had a previous injury or trauma to the area. In this blog post, we will discuss what causes posterior tibial tendonitis and how it can be treated. We’ll also go into detail on how long it takes to recover from posterior tibial tendonitis and how you can prevent future injuries or recurrences.
What is Posterior Tibial Tendonitis?
Posterior Tibial Tendonitis (PTT) is an overuse injury of the posterior tibial tendon located in the lower leg which runs from behind the inside of your ankle into the midfoot. It is responsible for supporting the arch of your foot and providing stability during movement. The muscle starts very deep in the back of the calf and eventually wraps around the inner ankle bone called the medial malleolus and eventually attaches to a bone called the navicular tuberosity and the inner part of the arch. Posterior tibial tendonitis develops when the tendon becomes inflamed due to overuse or trauma from a fall or other type of accident. Symptoms include pain near your inner ankle bone that worsens with activity, swelling, difficulty walking barefoot, soreness when pressing on the inside of your ankle bone, and feeling like your foot is going numb or weak when standing for long periods of time.
One of the major risk factors for posterior tibial tendinitis is flatfoot deformity. The posterior tibial tendon is a important structure that helps stabilize the arch. If an individual already has a lower arch, the posterior tibial muscle and tendon has to work even harder to try and support the arch. That is why it is common to see the posterior tibial tendon issues in people that have flatfoot deformity. It is kind of like a chicken versus egg argument as to what came first. Sometimes having a flatfoot initially can lead to posterior tibial tendinitis. In some individuals, it is possible to start with a posterior tibial tendinitis which leads to more profound injury to the tendon with tearing and possible rupture, and this can eventually lead to flattening of the arch.
There are a variety of classifications for how bad the injury is to the tendon and how significant the flatfoot deformity is. The grade of injury will increase as degeneration, and disease to the tendon increases. It is also possible to see increased injury to the tendon with more advanced cases of flatfoot deformity. Treatment will depend on severity of the injury to the tendon. Earlier stages of injury are much easier to treat than advanced cases of injury. Earlier cases of injury will typically respond much better to bracing, orthotics and physical therapy. More advanced cases of posterior tibial tendinitis may require advanced regenerative options like radial shockwave treatment or PRP injections. If conservative treatment fails, you may need to consider a surgical repair of the tendon which typically will be performed in combination with a flatfoot reconstructive surgery.
How to decide between a custom orthotic and a brace for inner ankle pain?
A custom orthotic is a functional devices placed into the shoe to help support the arch. This can be highly beneficial with posterior tibial tendinitis, especially with significant arch pain as well. The way these devices work is by trying to put the foot into a better position biomechanically, and may help splint the foot so that the posterior tibial tendon does not have to fire as much. If the flatfoot deformity is so significant, especially if there is ankle involvement, typically a brace has to be considered because there is not enough control from a simple orthotic. Braces do not have to be bulky and they will typically fit into regular sneakers.
Regenerative options for posterior tibial tendinitis
Two options to consider that are regenerative for posterior tibial tendinitis would be either shockwave therapy or PRP injections. Shockwave is a noninvasive modality that works by introducing high-energy sound waves into the tissue to induce microtrauma. This new trauma reactivates the inflammatory cascade to increase blood flow, growth factors and healing of the tissue. Another exciting modality is platelet rich plasma injections. PRP works by obtaining a sample blood from the patient’s arm. The blood is then spun down in a centrifuge and the platelets are extracted from the sample and then reinjected back into the patient at the site of pathology. Both these options are highly effective in the appropriate individual and are much safer than corticosteroid injections.
What kind of surgeries can be performed for inner ankle pain?
Surgery can be considered if the patient has failed respond to a satisfactory course of conservative treatment options. An MRI will be very beneficial before considering surgery as this will help with surgical planning. The MRI can be useful for assessing how much injury has occurred to the posterior tibial tendon. MRI will offer a lot more information than an x-ray because you can actually see soft tissues and tendon with an MRI. The MRI will allow for easy identification of the posterior tibial tendon, whether it is thickened, degenerated with partial tears or if it is completely torn.
Surgery can be performed to remove the diseased portion of the tendon and to repair through a process known as retubularization. Sometimes the tendon cannot be salvaged and in these scenarios typically a tendon transfer needs to be performed. The most common tendon that is utilized for this purpose is the tendon right next to the posterior tibial tendon called the flexor digitorum longus. The flexor digitorum longus ultimately attaches to all 4 of the lesser toes to cause flexion of them. The flexor digitorum longus tendon is detached around the middle part of the foot and is anchored into the navicular. As such, it is converted from a tendon that causes flexion of the toes to a tendon that takes over function of the posterior tibial tendon to allow it to support the arch.
Isolated tendon procedures are typically not performed. They normally need to be performed in combination with other procedures like realignment of bone procedures, like with the heel bone. Another important feature of a flatfoot deformity would be contracture of the calf muscle. This must be addressed through a calf muscle lengthening procedure known as a gastrocnemius recession procedure.
It is clear that there are numerous methods to treat inner ankle pain and posterior tibial tendinitis. An individualized treatment plan must be tailored for each patient based on the severity of their condition whether surgical or conservative. To create the ideal care plan for each patient, it is essential to begin with a thorough history and physical exam. By combining this information with all imaging studies available, we can collate the data to craft an individualized treatment approach that helps patients reach their desired outcome.
Remember that prompt treatment will always yield best results so seek medical attention immediately if needed – good luck!